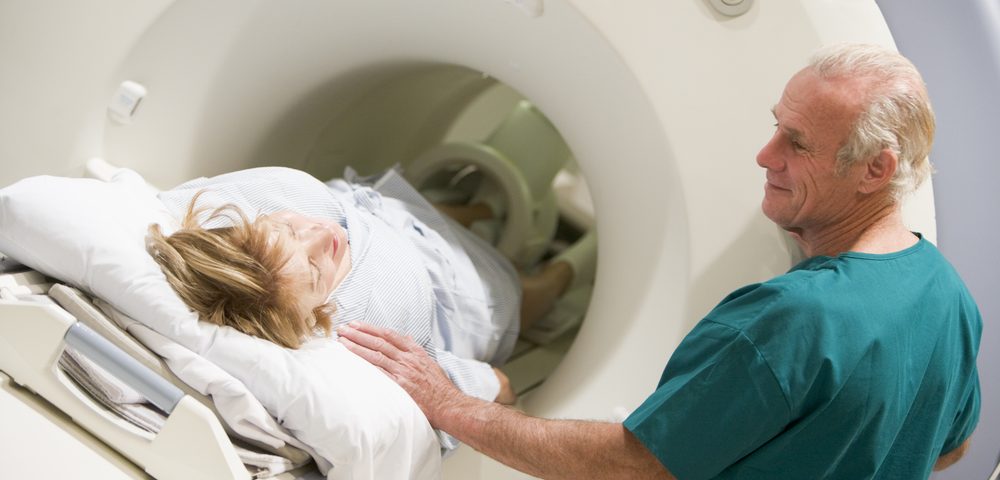
Despite no proven benefits for patients with ovarian cancer in remission, CT scans and cancer antigen 125 (CA-125) tests are still being routinely used in ovarian cancer surveillance, according to a study published in JAMA Oncology.
The results of a clinical trial presented at the American Society of Clinical Oncology (ASCO) Annual Meeting in 2009 had shown that CA-125 testing does not extend survival but increases the use of chemotherapy and decreases patients’ quality of life.
CT (computed tomography) scans are widely used in various medical contexts for diagnostic and monitoring purposes. The radiation used in CT scans can damage cells and have detrimental effects. CA-125 is a biomarker that may be elevated in the blood of some patients with ovarian and other types of cancers. The CA-125 is the most frequently used test to detect ovarian cancer.
To evaluate the clinical impact of the results presented at the ASCO meeting, authors of the recent study “Ovarian cancer surveillance with CA-125 tests, CT scans common despite lack of proven benefit,” examined the use of CA-125 testing and CT scans in clinical practice before and after 2009.
The analysis included more than 1,000 women with ovarian cancer who were in clinical remission following surgery and chemotherapy. The results showed no significant differences in the percentage of women who underwent three or more CA-125 tests, or in the percentage of women who underwent more than one CT scan before and after 2009.
There were also no significant differences in the time to re-treatment with chemotherapy before and after 2009 among women whose CA-125 markers doubled.
The researchers concluded that the recommendation to avoid routine surveillance testing has not been adopted into clinical practice.
“Although the routine use of CT scans has been strongly discouraged by guideline committees, CT scans appear to be routinely used, at significant cost,” Dr. Katherine M. Esselen, instructor of obstetrics and gynecology at Harvard Medical School and gynecologic oncologist at Beth Israel Deaconess Medical Center, and colleagues wrote in the study. “Future studies should examine which patient populations benefit most from surveillance testing to improve the value of cancer care.”
An analysis using 2015 Medicare reimbursement rates calculated the cost of the tests to be more than $16 million per year.
In a commentary accompanying the article, Dr. James S. Goodwin, chair of geriatric medicine in the department of internal medicine at University of Texas Medical Branch, wrote: “In an era of increased shared decision-making, patients’ desires for more information likely contributed to the continued use of surveillance testing, but why would clinicians present the option of CA-125 testing? Shared decision-making does not require that physicians present the patient with harmful options. We do not discuss heart transplants with patients who have mild congestive heart failure. Why would we discuss CA-125 testing with women who have ovarian cancer in remission.”
The Society of Gynecologic Oncology (SGO) classified CA-125 testing as optional, but it recommended against routine imaging for ovarian cancer surveillance as part of the Choosing Wisely campaign, an initiative of the American Board of Internal Medicine (ABIM) Foundation launched with the goal of advancing a national dialogue on avoiding wasteful or unnecessary medical tests, treatments, and procedures.